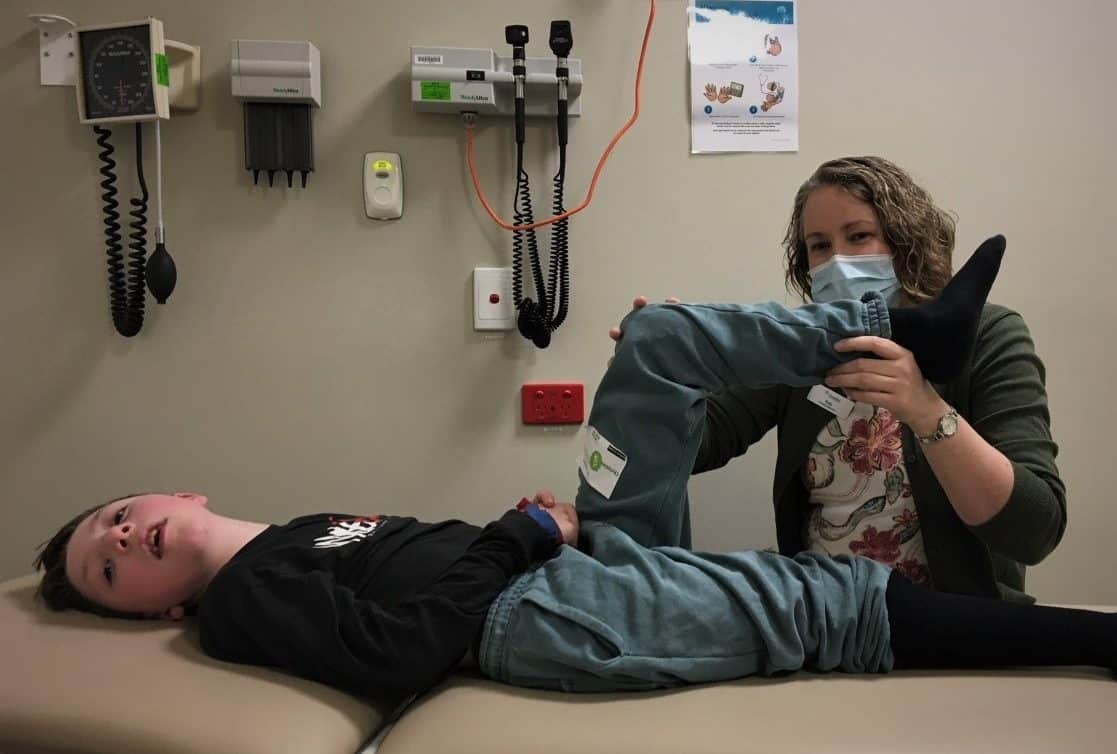
Every year around 120 children in Victoria are diagnosed with cerebral palsy (CP). For those with limited mobility, hip displacement can emerge as a serious medical issue.
As children with CP grow, the hip joint can change shape with the ball moving out of the socket over time. If the hip joint reaches the point where it dislocates, there can be serious problems with movement, sitting ability and pain.
“Many of the children who develop dislocated hips experience pain that can be unrelenting,” says Professor Dinah Reddihough, Principal Research Fellow at the Murdoch Children’s Research Institute.
“If it’s not picked up early, these young people may require complex and invasive surgery that can have limited effectiveness in reducing symptoms.”
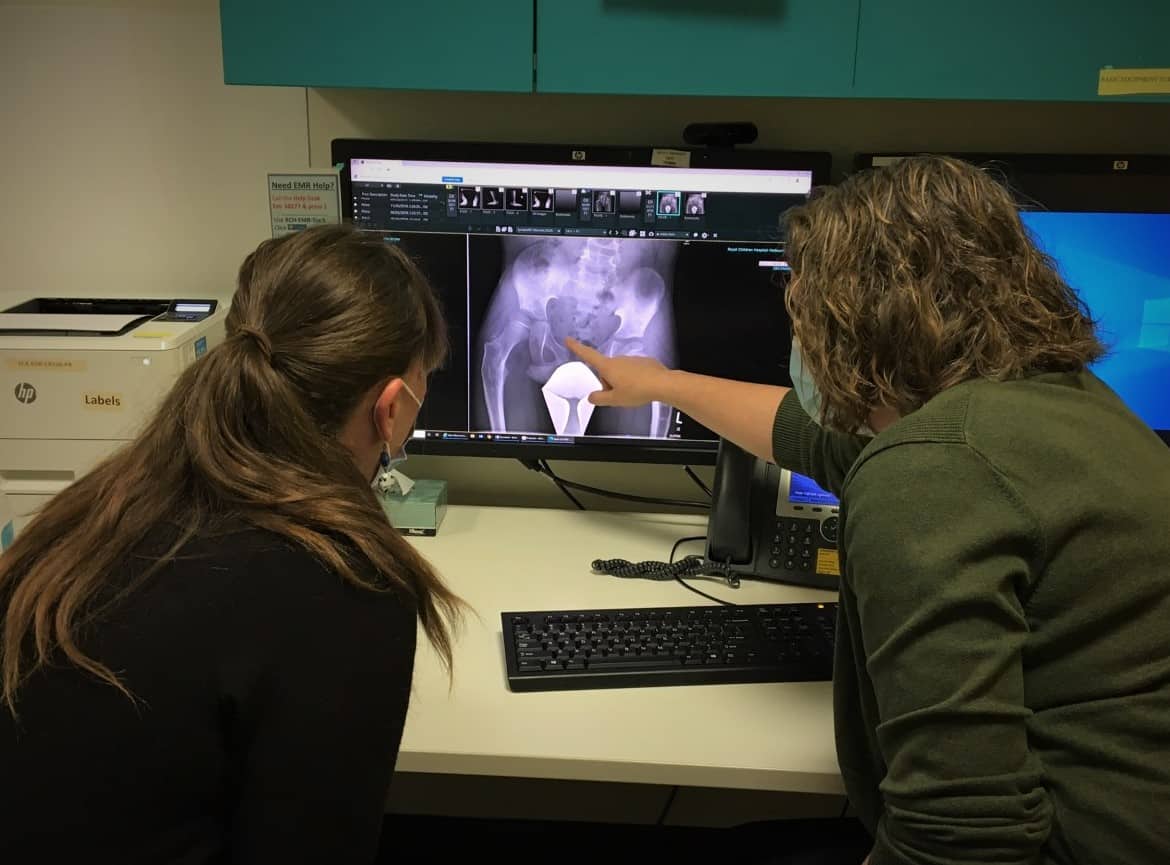
Fortunately, if the issue is identified early before the displacement is too severe, it can be addressed with more effective surgery. Regular X-rays are the only way to monitor the development of a child’s hips, but in some cases these can be missed by both clinicians and parents.
“Parents of children with CP, and the clinicians that support them, often have so many things to manage,” says Dr Kate Willoughby, physiotherapist at the Royal Children’s Hospital and Postgraduate Research Fellow researcher at the Murdoch Children’s Research Institute.
“They might be dealing with respiratory illness, seizures and all sorts of other acute medical issues. Managing all of these medical comorbidities is challenging for everyone. Hip displacement is important, but it is only one of the many potential medical issues that need to be on a clinician’s radar.”
National clinical guidelines for hip surveillance have been published since 2008, but preliminary research conducted by Dr Willoughby and her team identified a wide range of barriers that might prevent or delay a child’s hip surveillance. These barriers range from challenges in identifying which clinician is responsible for organising the X-ray, to it simply being forgotten among other, more immediate issues.
Making sure these regular X-rays happen is the goal of ‘HipWatch’, a new state-wide hip surveillance network that will be rolled out across Victoria. This MACH-supported project is funded by the Australian Government’s Medical Research Future Fund (MRFF) as part of the Rapid Applied Research Translation program.
Best practice
HipWatch, led by Dr Willoughby, is designed to address current barriers and improve efficiency in the implementation of hip surveillance. Their goal is that no Victorian child with CP is missed.
A customised database will enable centralised data collection and be linked to the Victorian Cerebral Palsy Register.
This will facilitate all children with CP in Victoria being enrolled in the program, identify when a child is due for a check, and enable their clinicians to be kept up to date with the results of hip surveillance X-rays.
The service will make sure children are having X-rays when they need them, but also ensure they aren’t receiving too many.
“The problem can go in two directions,” says Dr Willoughby.
“Children with CP can have multiple clinicians involved in their care. It can be easy for someone to assume that another clinician is taking responsibility and an X-ray can be missed. But some children can end up having double x-rays because everyone is so keen to make sure they’re done.”
Another challenge is that different children need X-rays at different times. Children who walk independently are far less likely to develop hip displacement, and as such require fewer checks. Children who are not able to walk can require X-rays as frequently as every six months.
“If it were a one-off screening X-ray the process would be much easier, but we need many children with CP and their parents to remain engaged in regular hip surveillance up until their adolescent or young adult years,” says Dr Willoughby.
Streamlining care
The HipWatch database is currently under development and is being tested by clinicians. Their feedback will be implemented into its design ahead of a wider clinical rollout.
One of the key collaborators of Hips on Track is the Victorian Paediatric Rehabilitation Service, which operates hubs in suburban and regional centres. Connecting these hubs with a central coordinating service through the database will be a key aspect of HipWatch.
“That central location will record not just the data from the X-rays, but also which team is currently taking responsibility for the child’s X-rays,” says Dr Willoughby.
HipWatch will be led by two Coordinators, based at the Royal Children’s Hospital and Monash Children’s Hospital.
Over the past 2 years, Dr Willoughby has piloted a physio-led clinic at the Royal Children’s Hospital along with other activities to support clinicians in implementing hip surveillance. As part of HipWatch, her role will be mirrored at the Monash Children’s Hospital to help the service reach more children and clinicians across the state.
The project is also aiming to improve knowledge about hip surveillance.
“Over the past few months around 100 clinicians and 250 families have responded to surveys about hip surveillance so that we can identify knowledge gaps and learning needs,” says Dr Willoughby
We also asked them about the methods they prefer to use to learn more about hip displacement,” says Dr Willoughby.
“To receive so many replies to the survey has been amazing, and we’ll be using the responses develop a range of resources to share information with parents and clinicians about hip displacement and the surveillance process.”
The team hopes these combined efforts will improve implementation and understanding about hip surveillance among both the parents of children with CP and the clinicians who support them.
Professor Reddihough says the HipWatch program will have a significant impact on outcomes for children with CP.
“We’re making sure children get the right hip X-rays at the right time, with the right referrals to the orthopaedic specialists when needed, so we don’t get into the state we were in 20 years ago when we had more children with dislocated hips and in severe pain.”
Read more on the Hips on Track project page.